A sudden fall or a significant blow can result in a painful and debilitating injury to the shoulder called a proximal humerus fracture. This common injury affects the upper part of the arm bone, or humerus, near the shoulder joint. It often demands careful evaluation and a personalized approach to healing. Understanding your injury and the available options for proximal humerus fracture treatment is an important step toward a successful recovery.
Key Takeaways
- The best treatment approach for proximal humerus fractures depends heavily on the fracture pattern, your age, and your overall health and activity level.
- Many proximal humerus fractures are minimally displaced and successfully heal with immobilization, pain management, and a structured physical therapy program.
- Surgical intervention may be recommended for severe or displaced fractures. Options may involve plates and screws (ORIF) or a shoulder replacement (arthroplasty).
Understanding the Proximal Humerus
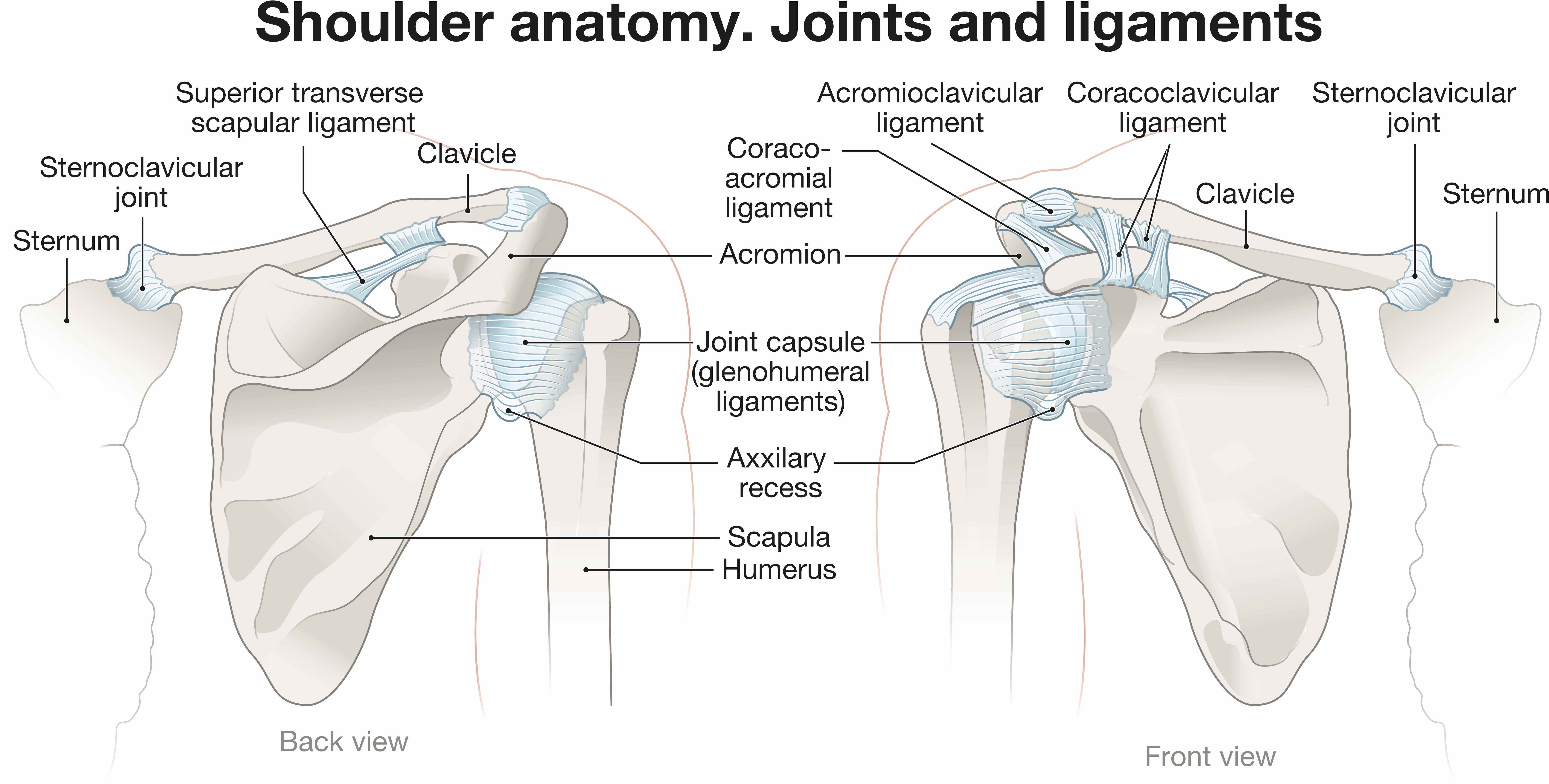
The shoulder is a complex and mobile joint, allowing for a wide range of motion. The proximal humerus is the rounded top section of the arm bone that fits into the shallow socket of the shoulder blade, which is called the glenoid. This arrangement forms the ball-and-socket joint. Several important structures attach to this area, including the rotator cuff tendons, which support lifting and rotating the arm.
The proximal humerus has four main parts that can fracture: the head (the ball), the greater tuberosity (where three of the rotator cuff tendons attach), the lesser tuberosity (where the fourth rotator cuff tendon attaches), and the shaft (the long part of the bone). When a fracture occurs, the break can involve one, two, three, or all four of these segments. The number of fractured parts and how far they have moved from their normal position significantly influences the recommended treatment path.
Causes and Risk Factors for Fractures
The most frequent cause of a proximal humerus fracture is a simple fall onto an outstretched arm. This mechanism is particularly prevalent in older adults. In this population, the primary risk factor is osteoporosis, a condition that causes bones to become weak and brittle. A fall that might only cause a bruise in a younger person can result in a fracture in someone with diminished bone density.
Conversely, younger, more active individuals typically sustain these fractures from high-energy trauma. Examples of high-energy trauma include motor vehicle accidents, falls from a significant height, or sports-related injuries.
Other factors that may increase your risk include certain medical conditions that affect bone strength, such as metabolic disorders. Additionally, a sedentary lifestyle can contribute to poor balance and muscle weakness, increasing the likelihood of a fall. Taking steps to improve bone health and prevent falls may help reduce the risk of this type of injury.
Diagnosis: What to Expect
If you experience a proximal humerus fracture, you will likely feel immediate, intense pain. You may notice swelling and bruising around the shoulder and upper arm. Moving the arm becomes extremely difficult, if not impossible. Bruising can sometimes travel down the arm and even reach the chest or hand over the next few days.
When you seek medical attention, the doctor will first perform a physical examination. They may carefully assess your shoulder, looking for signs of deformity and checking your skin for any open wounds. The doctor may also check your circulation and nerve function in the arm and hand.
Imaging studies may be used to support the diagnosis and determine the fracture pattern. Standard X-rays, taken from several different angles, allow the orthopedic specialist to see how many parts of the bone are broken and how far the pieces have separated or rotated. In some cases, especially if planning for surgery, your doctor may order a Computed Tomography (CT) scan. A CT scan provides a detailed, three-dimensional view of the fracture. This detailed image may help the surgeon better understand the complexity of the break.
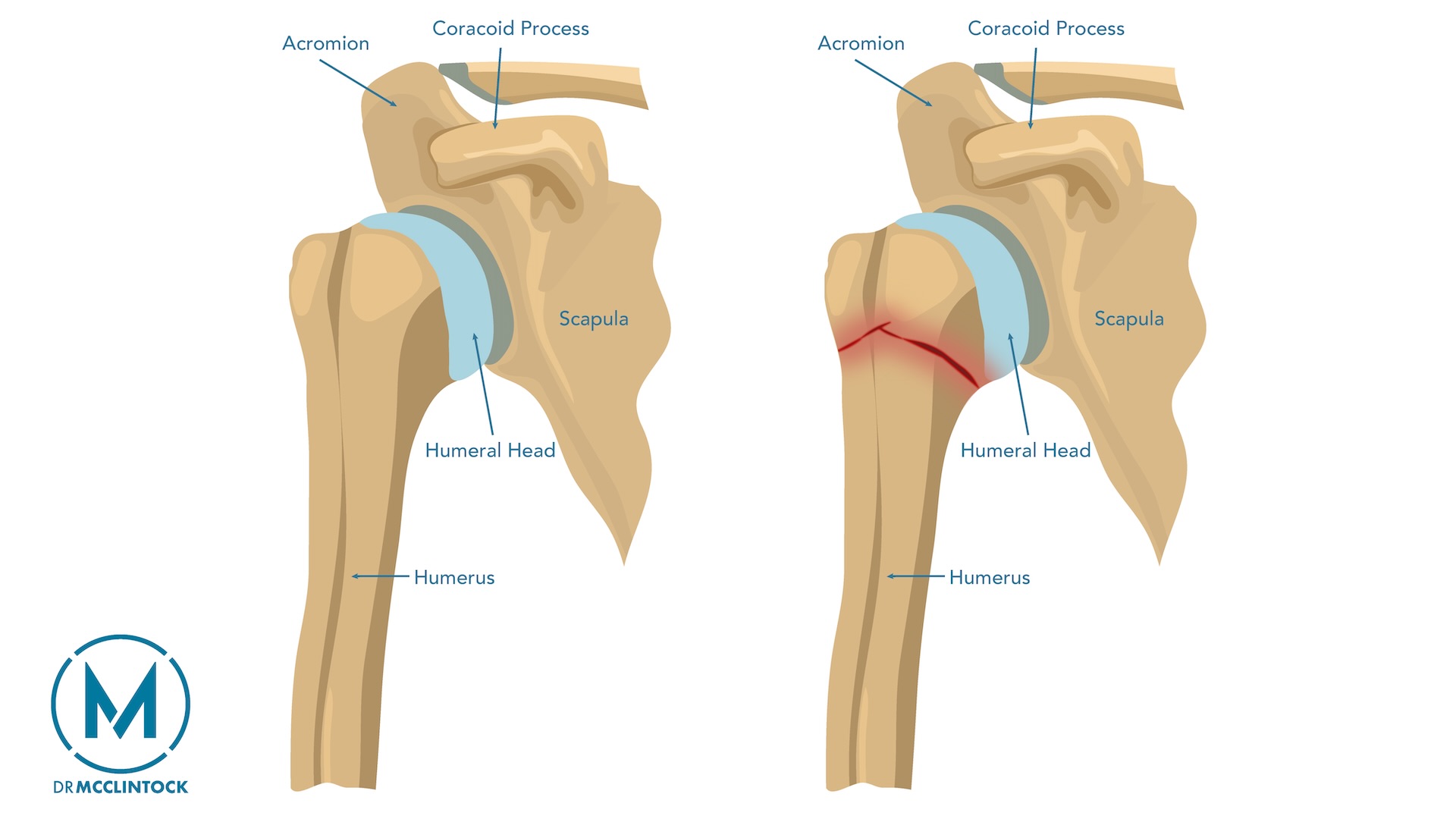
Proximal Humerus Fracture Treatment
The decision between non-surgical and surgical proximal humerus fracture treatment is not a one-size-fits-all choice. It involves a careful, individualized assessment of several key factors. An experienced orthopedic specialist will consider the characteristics of the fracture itself, as well as your personal health profile and lifestyle goals.
Factors Influencing the Treatment Choice:
- Fracture Pattern: The stability and displacement of the fracture fragments are key factors. Minimally displaced or stable fractures often respond well to non-operative care. Conversely, fractures that are significantly displaced, unstable, or involve multiple fragments may require surgery to restore alignment and function.
- Patient Age and Bone Quality: Older patients, particularly those with poor bone quality (osteoporosis), may have difficulty holding surgical implants. However, they may also benefit from a shoulder replacement if the fracture is severe. Younger, active patients with good bone quality may be more likely to undergo a procedure aimed at fixing and preserving their natural joint.
- Overall Health and Activity Level: A patient’s general health status, including any other medical conditions, can influence their ability to tolerate surgery and the intensity of post-operative rehabilitation.
- Rotator Cuff Involvement: If the fracture involves the greater tuberosity and the rotator cuff tendons are pulled out of place, surgery may be recommended to reattach the tendons and restore shoulder mechanics.
Your doctor will discuss these factors with you, explaining the risks and benefits of each approach.
Non-Surgical Treatment: When Less is More
Many proximal humerus fractures are minimally displaced or stable enough to heal without surgery. This approach relies on the body’s natural ability to repair bone, supported by external immobilization.
The Non-Surgical Protocol:
- Immobilization: You may wear a sling or a specialized shoulder immobilizer for a period of time. The sling holds the arm close to the body and prevents movement at the fracture site.
- Pain Management: Pain control is a priority during the initial phase. Your doctor will advise on appropriate pain medication. Applying ice packs to the shoulder can also help reduce swelling and discomfort.
- Early, Gentle Motion: While the fracture needs time to heal, the shoulder joint itself can quickly become stiff. Your doctor or physical therapist will guide you through gentle, passive range-of-motion exercises to prevent stiffness.
- Progression to Active Motion: Once cleared, you may progress to active range-of-motion exercises. At this stage, you start using your own muscles to move the arm. The physical therapist may guide you through a structured program to gradually restore movement and then begin strengthening the muscles around the shoulder.
Surgical Treatment Options
When a fracture is significantly displaced, unstable, or involves the joint surface in a way that threatens the blood supply to the bone, surgery may be recommended. The choice of surgical procedure depends on the fracture pattern, the quality of the bone, and the patient’s age and functional demands.
Open Reduction and Internal Fixation (ORIF)
ORIF is a common surgical approach for displaced proximal humerus fractures, especially in younger patients with good bone quality. The surgeon makes an incision to access the fracture site. They carefully manipulate the bone fragments back into their correct anatomical position. Once aligned, the fragments are held in place using specialized orthopedic hardware, typically a metal plate and screws.
Shoulder Arthroplasty (Joint Replacement)
For more complex fractures, particularly those where the blood supply to the humeral head is compromised, a shoulder replacement may be proposed. This is especially true for older patients with poor bone quality.
A reverse shoulder replacement is increasingly recommended as a surgical treatment for complex proximal humerus fractures in older patients. In a reverse replacement, the ball and socket are switched: a metal ball is fixed to the shoulder blade (glenoid), and a plastic socket is placed on the upper arm bone (humerus). This reversal changes the biomechanics of the shoulder. It allows the deltoid muscle, rather than the damaged rotator cuff, to power the arm’s movement. This is an advantage when the rotator cuff is either irreparable or damaged by the fracture.
Summary
A shoulder fracture can be a significant injury, but modern orthopedic care offers a range of proximal humerus fracture treatment options. Whether your injury is managed non-surgically with a sling and physical therapy, or surgically with internal fixation or a shoulder replacement, the path to recovery is a collaborative effort. We encourage you to maintain an open dialogue with your orthopedic specialist to ensure your treatment plan aligns with your specific injury and your personal goals for returning to an active, fulfilling lifestyle.
Frequently Asked Questions
What is the difference between a total shoulder replacement and a reverse total shoulder replacement for a fracture?
A standard total shoulder replacement is rarely used for fractures and mimics the natural anatomy of the shoulder. A reverse total shoulder replacement is often preferred for complex fractures in older patients because it reverses the ball and socket, allowing the deltoid muscle to power the arm, which is beneficial if the rotator cuff is damaged.
Is it normal to have bruising travel down my arm?
Yes, it is common. The blood from the fracture site can track down the arm due to gravity, causing bruising that may extend down to the elbow or even the hand.
When can I return to sports or heavy lifting?
Returning to high-impact sports or heavy overhead lifting is a gradual process. Depending on the injury, it usually requires several months of intensive strengthening. Your doctor may clear you to return only after assessing your strength and stability.