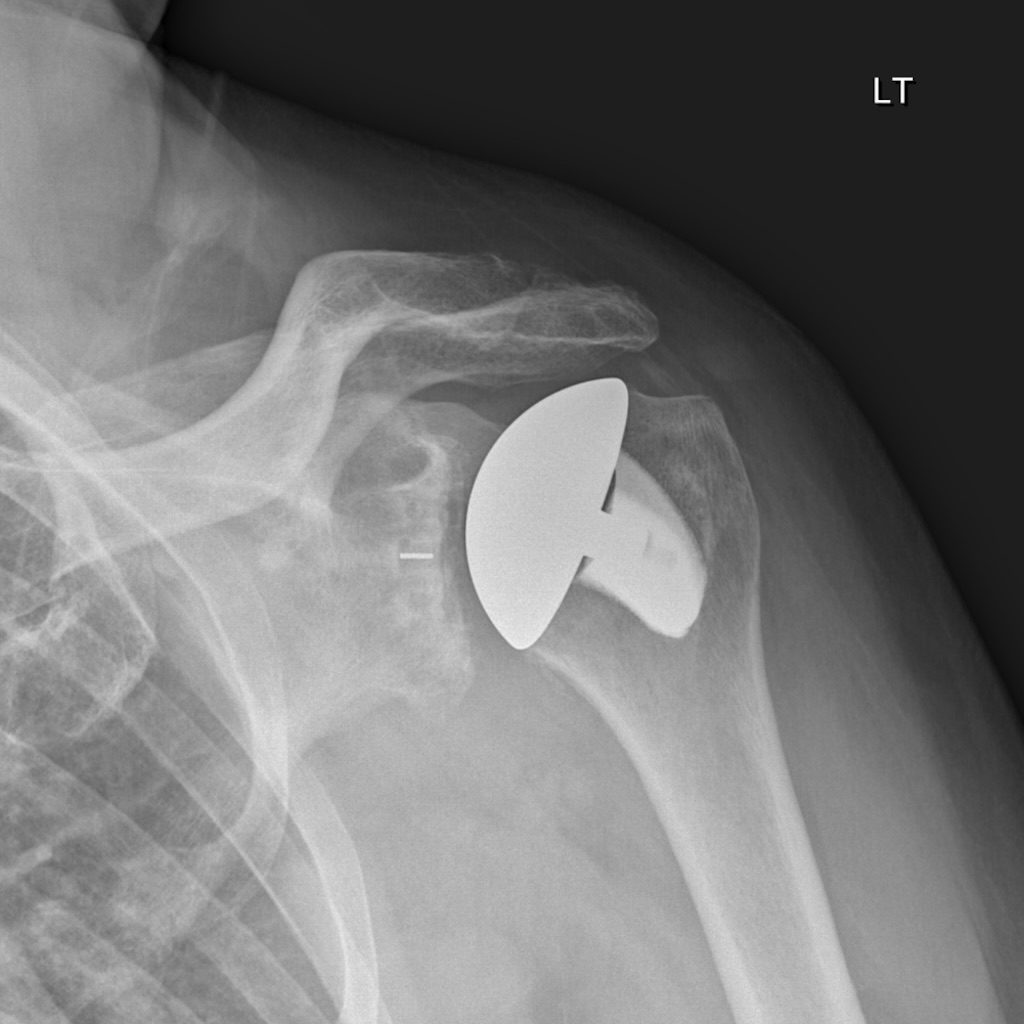
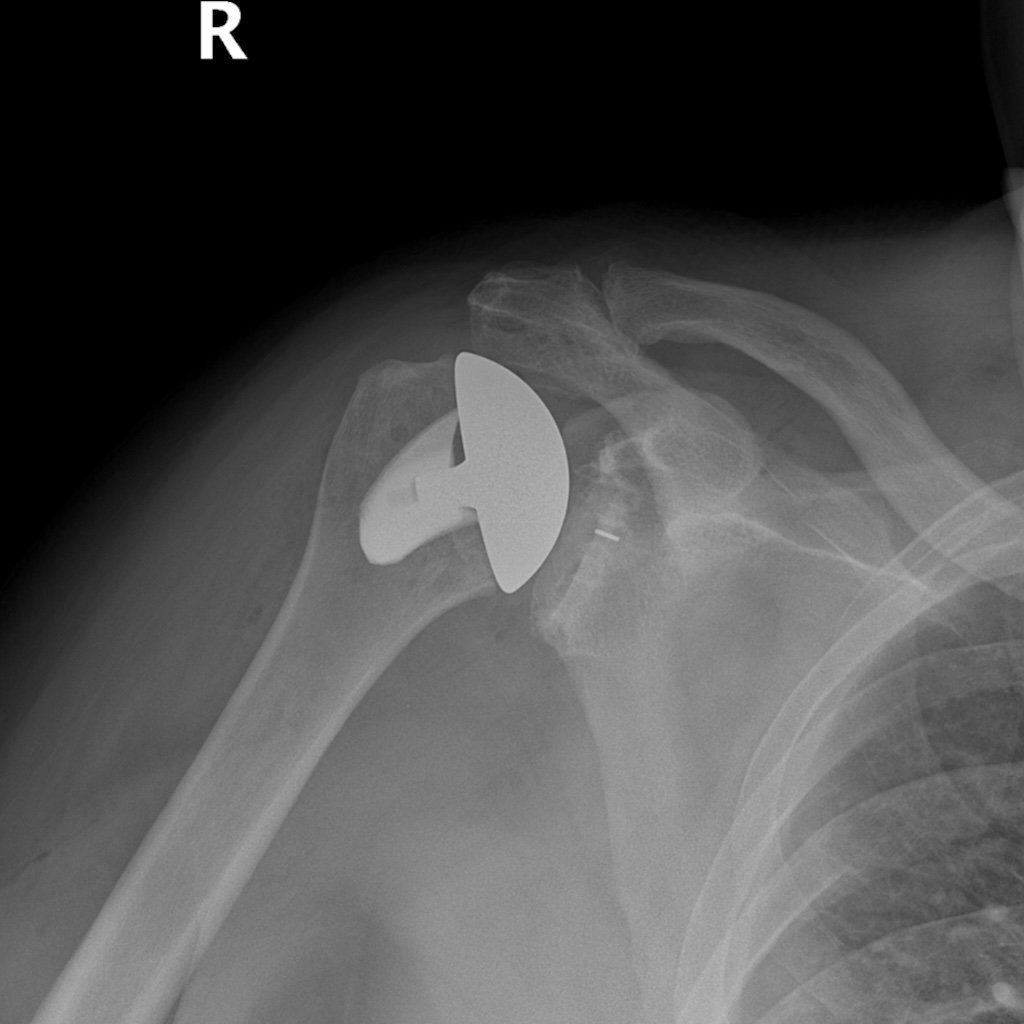
Total Shoulder Replacement
Shoulder replacement surgery is most often performed to relieve severe shoulder arthritis and restore pain-free motion. Dr. McClintock uses advanced 3D imaging, personalized surgical planning, and a conservative, patient-centered approach to help individuals return to their active lifestyles with long-lasting shoulder function.
584 N. Sunrise Ave.
Suite 140
Roseville, CA 95661
1625 Creekside Drive
Suite 200
Folsom, CA 95630
Dr. McClintock’s Services
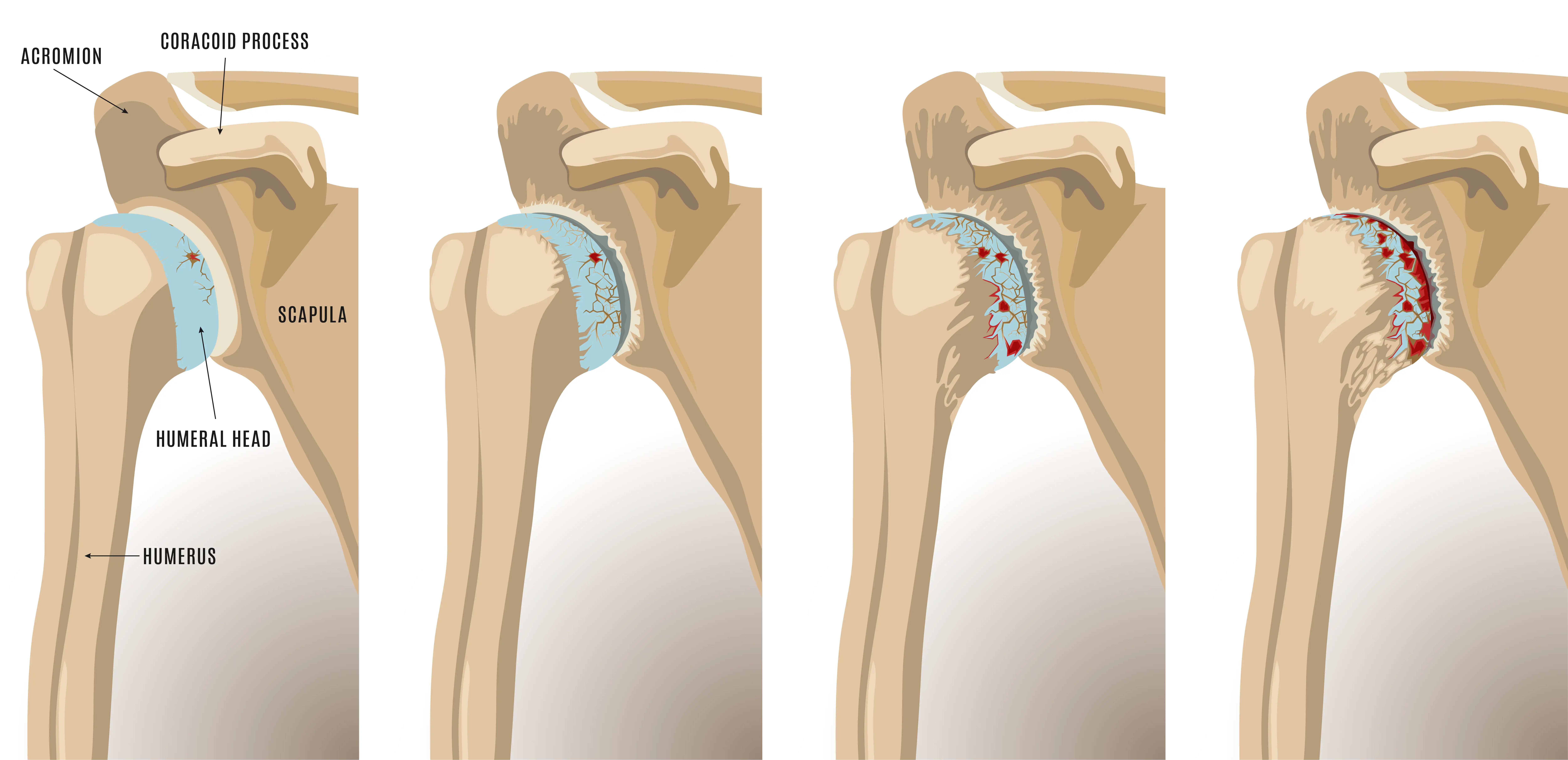
Conditions for Shoulder Replacement
The primary indication for total shoulder replacement surgery is glenohumeral arthritis. There are other indications for total shoulder replacement, including inflammatory arthropathy, posttraumatic arthritis, certain fracture scenarios, and others, but these are less common among the general population.
Shoulder Implant Technology
Shoulder implant technology has improved significantly over the years. The longevity of our implants is now excellent. As a shoulder surgeon, it has been exciting to see the evolution and the progression of the technology that helps people get back to their active lifestyles.
When Is It Time To See A Shoulder Specialist
I have two questions that I ask patients when they come to see me in the clinic:
1. Does it wake you up at night?
I think that’s a real problem that a lot of people with shoulder pain suffer from.
Whether it’s a rotator cuff problem, glenohumeral arthritis, or some other inflammatory condition of the shoulder, if the shoulder hurts at night, it’s time to see a specialist.
2. Are you able to do the things you love?
My whole philosophy on orthopedics, in general, is that I don’t save lives, I save lifestyles.
My goal is to get people back doing the things that they like to do. If you love golf and can’t swing your golf club, or if you like to play tennis and can’t go out and hit the court, then it’s time to get it looked at.
What to Expect In A Shoulder Appointment
To start, I want patients to come in and feel comfortable and give them the attention they deserve.
Getting to know patients as people really helps in terms of pinpointing the exact origin of their pain, and what we can do to treat it.
It’s important for me to fully understand things like:
- What symptoms are they experiencing?
- What type of lifestyle do they live from an activity standpoint?
- What do they do for employment?
- What are their hobbies and future goals?
Taking the time to really go through the important details together goes a long way in helping reach the best possible outcomes.
My Approach to Shoulder Replacement Surgery
Conservative Approach First
I think a lot of people tend to be a little nervous when they go to an orthopedic surgeon’s office. In general, I’m a fairly conservative practitioner when it comes to surgical indications. I really don’t like offering people surgery on the very first visit. I’m going to make sure that we’ve exhausted the conservative treatment options before we go down the path of surgery.
During the initial visit, we’ll spend time talking about shoulder anatomy, shoulder function, and reviewing their diagnosis. From there, we discuss things that we can do to alleviate pain without requiring surgery.
When Is It Time For Surgery?
I develop treatment plans according to the individual needs of each patient. Surgery is a last resort in almost every scenario. However, if the conservative treatment options don’t work, then it may be time to begin discussing shoulder replacement surgery as a potential option.
Key indicators for shoulder replacement are:
- Not getting good sleep due to shoulder pain at night
- Not being able to resume a normal lifestyle
- Not being able to get back to work
Failure of conservative treatments such as cortisone injections, physical therapy, NSAIDs, and other modalities.
In taking that approach, I want to make sure people feel comfortable and know that we are trying to do what’s best for them.
Shoulder Replacement Surgery – What to Expect Pre-Op
Planning the Surgery
As technology has improved, we’ve developed the ability to take CT images and use them to gain a better understanding of the three-dimensional geometry of each patient’s shoulder. I like to utilize these tools to assist in the surgical planning process.
I use the CT images and a surgical software program to map out each patient’s shoulder. This provides a customized preview for correctly positioning the implants to rebalance the shoulder. This allows me to plan the entire surgery before it even happens. That way, I’m able to provide a fully customized approach to each shoulder and maximize the likelihood of a good outcome.
Managing Any Existing Health Conditions
I also want to make sure that people are healthy in terms of their other medical comorbidities. Conditions such as diabetes, high blood pressure, or other cardiovascular or pulmonary issues must be well managed so that we can minimize any potential risks postoperatively.
Often this involves coordinating that care with the patient’s primary care physician to fine-tune any necessary adjustments before we embark on surgery.
What to Expect the Day of Surgery
It’s normal for people to be anxious on the day of surgery. Just know that, first and foremost, the staff at the facility are there to help take care of your needs, and are more than willing to answer any questions that you have. I always encourage patients to write down any last-minute questions so that we can talk before we go into the operating room.
Together in the pre-op area, I want to review all of the risks, goals, and objectives that we discussed in the office before surgery, and what we’re going to accomplish in the operating room. I do my best to answer any questions that patients and their families may have prior to the procedure. It’s important that each patient makes a fully-informed decision on their care.
Anesthesia for Shoulder Replacement Surgery
In the majority of shoulder replacement surgeries, we utilize regional anesthesia, in addition to general anesthesia. That involves a block where the anesthesiologist will place a numbing medication around the nerves that supply sensation to the upper extremity that we are operating on.
This approach helps reduce the amount of anesthesia required during the procedure, so that people wake up faster, with fewer side effects of the anesthesia, such as nausea and vomiting. It also helps with post-operative pain control immediately following the procedure.
Shoulder Replacement Surgery – Post Operative Appointments and Recovery
In my office, we do a lot to organize the recovery and the post-operative plan before the surgery.
Typically, the first post-op visit is 2 weeks from surgery, with follow-ups at 6 weeks and 12 weeks postoperatively. We take X-rays and check the range of motion to make sure that therapy is going well, and that there aren’t any issues or concerns that are developing.
Therapy begins around the 2-week mark, following the procedure. We help people progress through that treatment algorithm so that they can regain their motion and strength in the shortest amount of time possible.
Generally speaking, following a shoulder replacement surgery, patients will be in a sling for 6 weeks to allow healing of the soft tissues. Then we start active range of motion at 6 weeks and strengthening at 12 weeks.
In general, I tell patients that full recovery can take about 3 to 4 months. At 3 months post-op, most restrictions are lifted, and people can begin trying to adapt back to their lifestyle and try out their new shoulder!