If you have diabetes, you may face an increased risk of developing various shoulder conditions that can interfere with your daily activities and quality of life. Diabetic shoulder problems represent a group of musculoskeletal conditions that appear to occur more frequently in individuals managing diabetes than in the general population. Understanding these conditions can help you recognize symptoms early and seek appropriate treatment to maintain your shoulder function and overall wellness.
Key Takeaways
- Diabetes appears to increase the risk of developing several shoulder conditions, including frozen shoulder and rotator cuff tears.
- Elevated blood sugar levels may contribute to changes in connective tissue that affect shoulder mobility and healing.
- Treatment options typically range from conservative approaches like physical therapy to surgical interventions when necessary.
- Maintaining blood sugar control may help reduce the risk of developing diabetic shoulder problems in some cases.
The Diabetes-Shoulder Connection
The relationship between diabetes and shoulder disorders has been well-documented in medical literature, though researchers continue to explore the exact mechanisms behind this connection. When blood sugar levels remain elevated over time, they may cause changes in the body’s connective tissues, including those in and around the shoulder joint. These changes can affect the flexibility and strength of tendons, ligaments, and the joint capsule itself.
Glucose molecules may bind to proteins in a process called glycation, potentially altering the structure and function of collagen. Since collagen forms a major component of the tissues surrounding your shoulder, these changes can lead to stiffness and reduced mobility. Additionally, diabetes can affect blood flow and nerve function, which may impact healing processes and pain perception in the shoulder region.
Chronic inflammation associated with diabetes might also play a role in the development of shoulder problems. Inflammatory markers tend to be elevated in individuals with poorly controlled diabetes, and this inflammation can contribute to tissue damage and degenerative changes in the shoulder joint over time. The combination of these factors creates an environment where shoulder tissues may be more vulnerable to injury and less capable of efficient repair.
Common Diabetic Shoulder Problems
Frozen Shoulder (Adhesive Capsulitis)
Frozen shoulder represents one of the most common shoulder conditions associated with diabetes. This condition develops when the capsule surrounding the shoulder joint becomes thick and tight, restricting movement. Studies suggest that individuals with diabetes have a higher prevalence of frozen shoulder compared to the general population, with some research estimating rates several times higher.
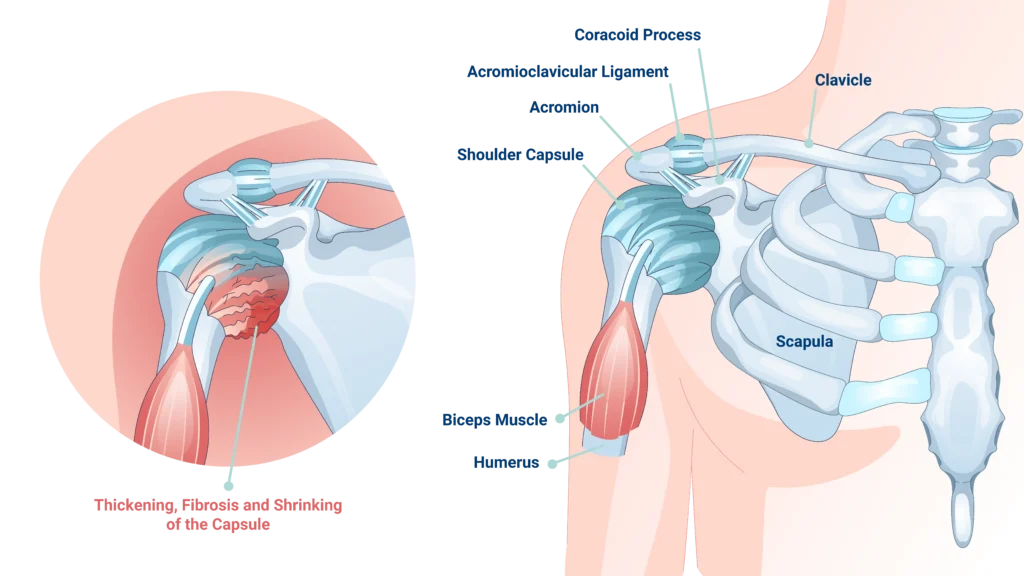
The condition typically progresses through three phases: freezing (gradual pain and stiffness), frozen (less pain but significant stiffness), and thawing (gradual improvement in mobility). During the freezing stage, you may experience gradually worsening pain and stiffness that can interfere with sleep and daily activities. The frozen stage follows, characterized by less pain but continued significant stiffness that limits your range of motion. Finally, the thawing stage involves gradual improvement in mobility, though this process can take many months or even years.
Rotator Cuff Disorders
The rotator cuff consists of four muscles and tendons that surround the shoulder joint, providing stability and enabling motion. Some studies have found an association between diabetes and a higher incidence of rotator cuff tears and tendinopathy. These tears can occur due to degenerative changes in the tendons or from acute injury.
Rotator cuff problems may be more common in individuals with diabetes, potentially related to changes in tendon structure, collagen quality, and impaired healing associated with chronically elevated blood sugar levels. The tendons may become less flexible and more prone to fraying or tearing with everyday activities. Even minor overhead movements that wouldn’t typically cause problems might lead to tendon damage in someone with long-standing diabetes.
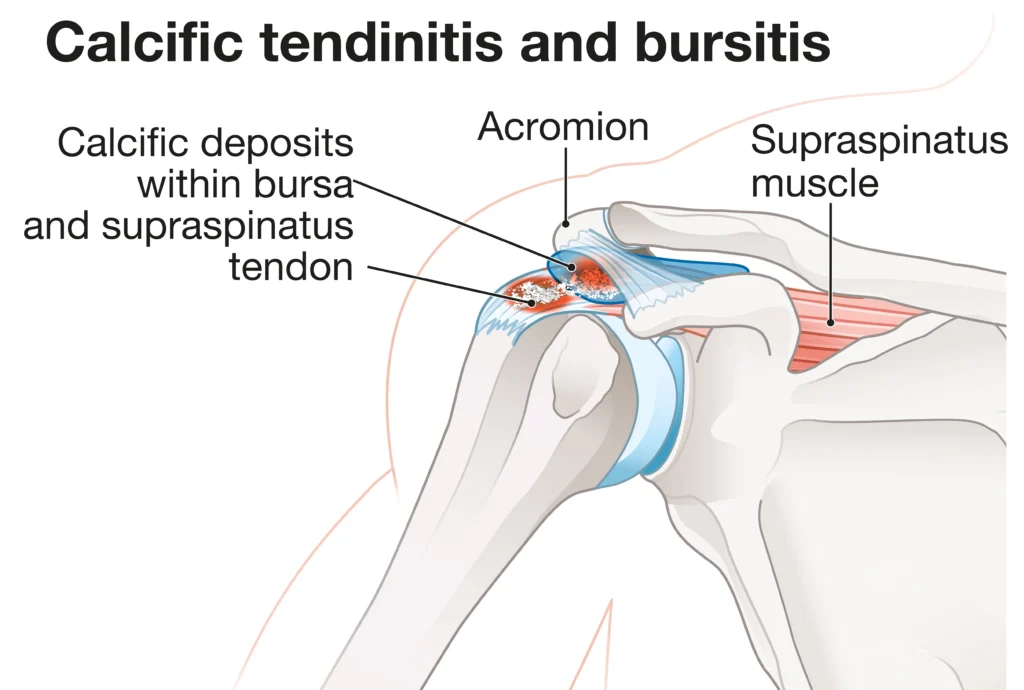
Calcific Tendinitis
This condition occurs when calcium deposits form within the rotator cuff tendons. While calcific tendinitis can affect anyone, some studies suggest an association between diabetes and increased prevalence. The deposits can cause inflammation and pain, particularly when they begin to break down and reabsorb. Symptoms range from mild discomfort to severe pain that disrupts sleep and daily activities. The deposits may appear on imaging studies and can sometimes resolve on their own, though treatment may be necessary in many cases.
Recognizing Symptoms
The symptoms of diabetic shoulder problems vary depending on the specific condition, but several common warning signs may prompt you to seek evaluation. Pain often represents one of the most frequent initial symptoms. This discomfort may start gradually or appear suddenly, and it may worsen with specific movements or at night.
Progressive stiffness makes it increasingly difficult to perform routine activities. You might notice difficulty reaching overhead, behind your back, or out to the side. Simple tasks like putting on a jacket, washing your hair, or reaching for items on high shelves may become challenging and frustrating.
Weakness can develop in the shoulder, particularly with rotator cuff problems. You may find it harder to lift objects or maintain your arm in certain positions. Some people describe a sensation of their shoulder “giving way” during activities.
Night pain frequently disrupts sleep, especially when lying on the affected shoulder, leading to fatigue and decreased quality of life. Some individuals also experience a catching or clicking sensation with shoulder movement, though this symptom isn’t universal across all shoulder problems.
Risk Factors Beyond Diabetes
While diabetes represents a risk factor, other factors may increase your likelihood of developing shoulder problems. People who have lived with diabetes for longer periods may face higher risks of developing shoulder complications, as the cumulative effects of elevated blood sugar take their toll on tissues over time.
Poor blood sugar control seems to correlate with increased rates of shoulder problems. Maintaining blood glucose levels within target ranges may help reduce your risk, though it doesn’t eliminate it entirely. Age also plays a role, with shoulder conditions becoming more common as we get older, regardless of diabetes status.
Other health conditions, such as thyroid disorders, can further increase risk. Previous shoulder injuries or surgeries may also make you more susceptible to developing additional shoulder problems.
Diagnostic Approach
When you visit an experienced orthopedic specialist for shoulder pain, the evaluation commonly begins with a discussion of your symptoms and medical history. Your doctor will want to know about your pain, when it started, what affects it, and how it impacts your daily activities.
A physical examination allows your doctor to assess your shoulder’s range of motion, strength, and tenderness. Specific tests help identify which structures might be involved.
Imaging studies often play an important role. X-rays can reveal bone changes, calcium deposits, and joint space narrowing. MRI provides detailed views of soft tissues, including tendons and muscles, which can be useful for identifying rotator cuff tears or other pathologies.
Treatment Options
Treatment for diabetic shoulder problems typically follows a stepwise approach, starting with conservative measures and progressing to more invasive interventions if necessary. Physical therapy is a treatment component for many shoulder conditions, aiming to help restore range of motion, build strength, and reduce pain.
Anti-inflammatory medications can help manage pain and reduce inflammation. Your doctor may recommend over-the-counter options depending on your symptoms. Corticosteroid injections may provide short-term relief for certain conditions by delivering anti-inflammatory medication directly to the affected area.
Platelet-rich plasma (PRP) injections represent a regenerative treatment option that may benefit some patients. This treatment uses components from your own blood to potentially promote healing.
When conservative treatments don’t provide adequate relief, surgical intervention may become necessary. For frozen shoulder, manipulation under anesthesia or arthroscopic capsular release can help restore motion. Rotator cuff tears may require surgical repair. Some surgical procedures can be performed arthroscopically, a minimally invasive method that may result in smaller incisions and shorter recovery times compared to traditional open surgery.
Prevention Strategies
While you cannot completely eliminate your risk, several strategies may help reduce it. Maintaining good blood sugar control represents one of the most important preventive measures.
Staying active and maintaining shoulder mobility through regular exercise can help keep your joints healthy. Gentle range-of-motion exercises and strengthening activities may help maintain mobility and reduce the likelihood of progressive stiffness.
Maintaining a healthy weight reduces stress on your joints. If you notice any shoulder pain or stiffness, don’t ignore it. Early evaluation and treatment may support better outcomes.
Summary
Diabetic shoulder problems encompass a range of conditions that appear to occur more frequently in individuals with diabetes compared to the general population. These conditions, including frozen shoulder, rotator cuff disorders, and calcific tendinitis, can impact quality of life through pain, stiffness, and functional limitations. The mechanisms linking diabetes to shoulder problems likely involve changes in connective tissue, altered healing processes, and chronic inflammation associated with elevated blood sugar levels.
Early recognition of symptoms enables timely intervention, which may improve outcomes and potentially prevent progression of mild conditions into more severe problems. Treatment approaches range from conservative measures like physical therapy and medications to surgical interventions when necessary.
Frequently Asked Questions
Why do people with diabetes get more shoulder problems?
Elevated blood sugar levels are associated with changes in connective tissue. Glycation of proteins may alter collagen properties, while reduced blood flow and chronic inflammation can impact healing. These factors may combine to increase susceptibility to shoulder conditions.
Can diabetic shoulder problems be prevented?
While complete prevention isn’t possible, maintaining good blood sugar control may reduce your risk. Regular exercise and avoiding repetitive overhead activities can also help. Early treatment of developing symptoms may help prevent progression.
Should I stop using my shoulder if it hurts?
Complete rest isn’t typically recommended. Gentle range-of-motion exercises often help prevent further stiffness, even with pain. However, avoid activities that cause severe pain. Your physical therapist can guide appropriate activity levels.