What is Reverse Shoulder Replacement Surgery?
Before the advantages of a reverse shoulder replacement can be fully understood, it’s important to grasp how the anatomy of your shoulder changes with this surgery.
The shoulder socket is made up of two parts: a ball at the top of the humerus (upper arm bone), which is tightly fitted to a concave, shallow depression on the scapula (shoulder blade bone) called the glenoid socket.
In a healthy shoulder, both the ball and the glenoid socket are covered with articular cartilage, a tissue that protects both bones and allows the joint to glide smoothly without damaging either bone or causing pain.
When a patient receives a reverse shoulder replacement, the position of the ball and socket is reversed. An artificial ball implant is attached to the scapula where the glenoid socket used to be, and an artificial socket is attached to the top of the humerus where the natural ball used to be.

Pros of Having Reverse Shoulder Replacement Surgery
Patients considering reverse shoulder surgery have often run out of other options for restoring function to their damaged shoulder. The biggest pro for this procedure is allowing patients to return to a normal, pain-free life. It restores function and allows for an active lifestyle again.
Reverse shoulder arthroplasties often have the most dramatic improvement from preoperative to postoperative function. Before surgery, reverse-candidate patients often have poor shoulder function, pain during everyday activities and are often up at night from shoulder pain.
Reverse shoulder replacements have a high success rate, and most patients can resume a normal lifestyle with full function within months afterward.
The primary reason a patient would benefit from a reverse shoulder replacement instead of a standard anatomic shoulder replacement is if the rotator cuff muscles are torn or damaged.
The Importance of Rotator Cuff Muscles
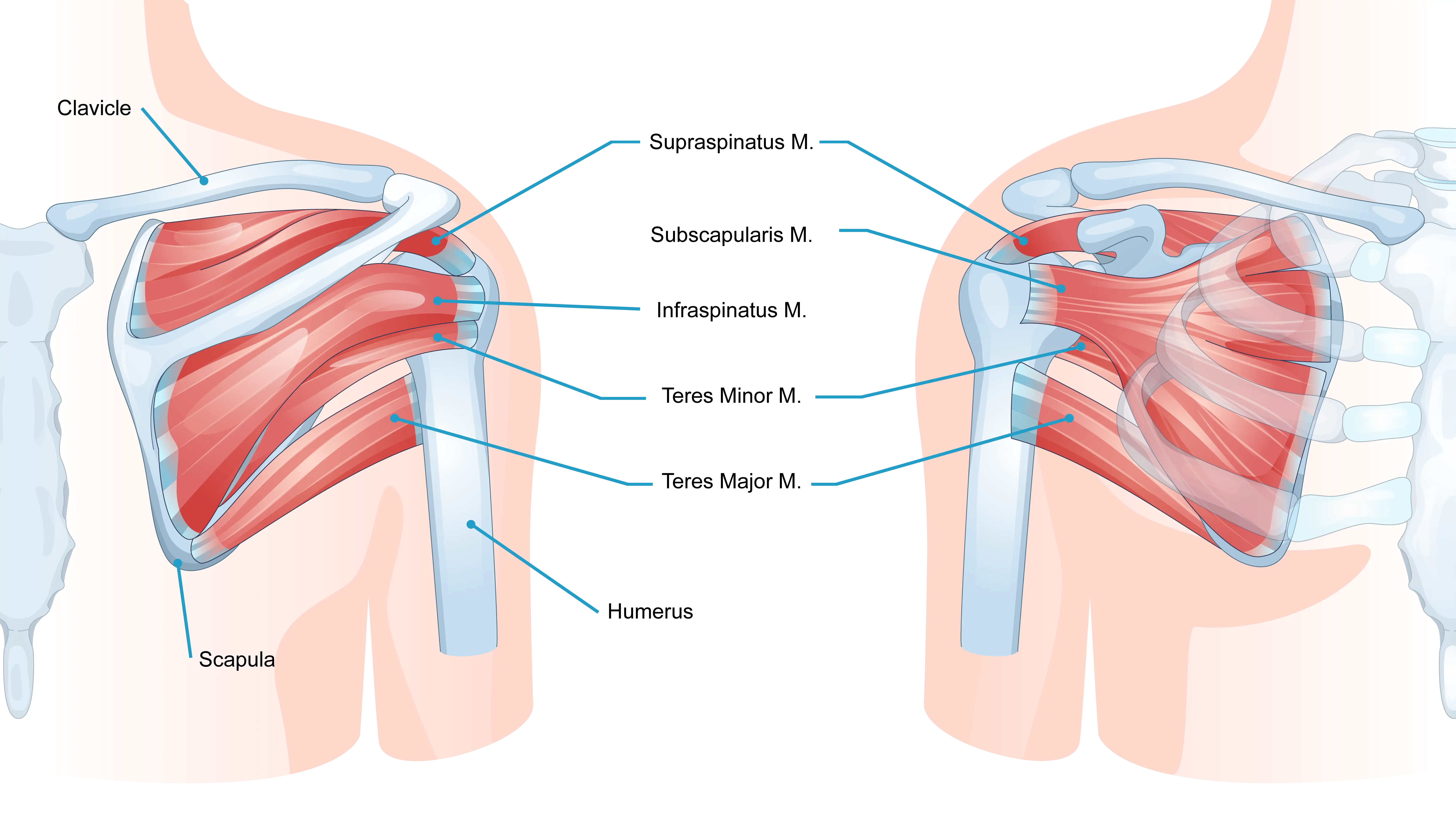
In a healthy functioning shoulder, the set of four muscles that form the rotator cuff holds the ball of the humerus tightly to the glenoid cavity, giving the joint stability and keeping the ball and socket in proper position. This prevents the shoulder from dislocating and causing pain and damage. The rotator cuff also gives the shoulder joint its wide range of motion.
Over time, the rotator cuff muscles can become torn or injured. When this happens, the tendons on the muscles no longer hold on tightly to the humerus head, and the joint becomes unstable.
In a traditional total shoulder surgery, called anatomic shoulder surgery, the ball of the humerus and the glenoid cavity are replaced by prosthetic components. This is effective when the only problem is disease and deterioration of the cartilage of the shoulder joint.
But if a patient has the additional problem of an ineffective rotator cuff, this will not be solved by simply replacing the diseased parts of the shoulder joint.
The design of the reverse implant itself overcomes many of the inherent deficits or weaknesses of the standard anatomic shoulder surgery.
Another Way to Gain Stability
Before reverse shoulder arthroplasty existed, there wasn’t a good way to regain shoulder stability for patients who had an irreparable rotator cuff.
But since 2004, reverse shoulder arthroplasty has been solving this problem very successfully. The surgery has now been around long enough for surgeons to see that it has very positive outcomes in patients long-term. Reverse shoulder surgeries have been rapidly expanding the ability of orthopedic surgeons to treat complicated pathology in the shoulder.
The number of reverse shoulder arthroplasties performed in the US is rapidly increasing due to the high success rates and excellent long-term viability.
Why Does Reverse Shoulder Replacement Surgery Work Where Anatomic Total Shoulder Surgery Does Not Work?
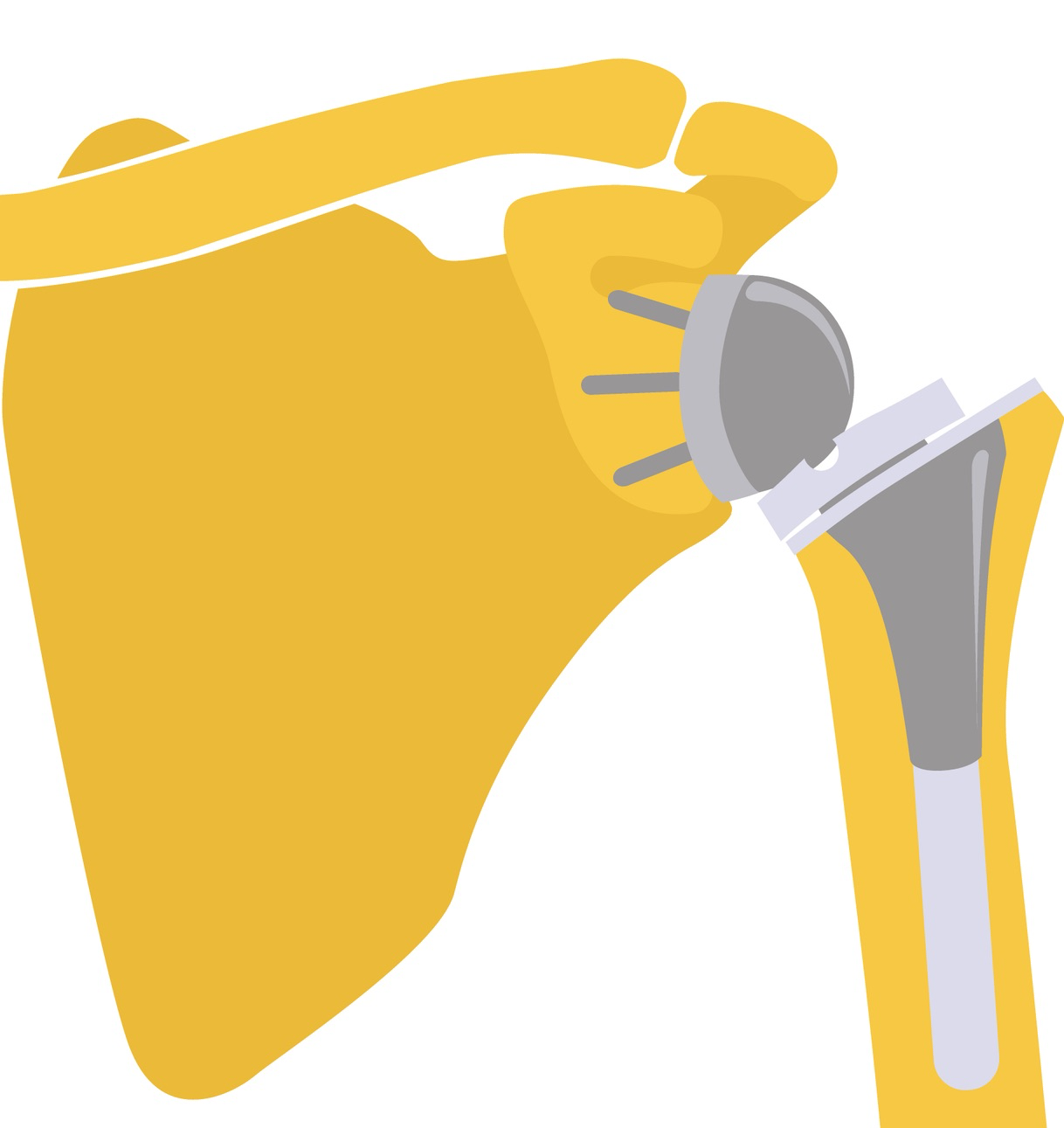
Reversing the anatomy of the shoulder means that there is no longer a large ball at the end of the humerus that the rotator cuff muscles must hold tightly in place. Instead, the ball portion of the joint is secured into the scapula with screws. This means that the deltoid muscles in the arm can now take over movement of the shoulder joint from the weak or injured rotator cuff.
Furthermore, the natural glenoid socket that the natural humerus ball fit into was very shallow and only slightly concave. This meant that all of the stability of the shoulder depended on the integrity of the soft tissues around the joint. But the manufactured implants for a reverse shoulder are a constrained design.
Reverse Shoulder Surgery could benefit you if you have:
- An irreparable rotator cuff tear
- Rotator cuff tear arthropathy (arthritis caused by joint instability)
- Internal derangement of the joint
- Chronic shoulder dislocation
- Poor shoulder function
- Failed anatomic shoulder replacement, which needs revision
- Complex deformities of the glenoid socket
- Proximal humerus fractures that can’t be reconstructed
- Tumor of the shoulder joint
- Difficulty lifting your arm over your head or away from your side and severe shoulder pain (pseudoparalysis)
- Have tried other methods of treatment like medications, rest, physical therapy, and cortisone injections that haven’t relieved the pain in your shoulder.
Cons to Reverse Shoulder Replacement Surgery
Reversing the anatomy of the shoulder presents some limitations.
Although many patients are thrilled that they can return to pain-free daily living, your shoulder may not feel exactly as it did when you were in your 20s. This is because the same mechanics that provide stability and eliminate pain slightly constrict the range of motion.
The goal of the reverse surgery is to restore function so that you can return to normal activities. But it is not designed to allow someone to be able to throw a baseball or football like they could when they were in college. It’s also not designed to enable heavy lifting.
Younger patients may be more disappointed with the mechanical limitations of their new shoulder. Patients in their 60s and above usually find it more than adequate for their lifestyle.
Some limits that patients experience have to do with internal rotation reduced strength when lifting overhead, and being able to reach behind the back. These will all be significantly improved from what the patient could do right before surgery but will be limited compared to what he or she was able to do when they were younger.





